Pressure ulcers (also called pressure sores or bedsores) are areas of skin and tissue damage caused when someone stays in one position for too long. They can be painful, serious, and even life‑threatening if they are not spotted and treated early.
Everyone working in care has an important role in preventing them, especially when supporting people in their own homes.
Who Is Most at Risk?
A person is more likely to develop a pressure ulcer if they:
- Have limited mobility or spend long periods sitting or lying down
- Are incontinent or have regularly wet/delicate skin
- Have reduced feeling in part of their body
- Can’t communicate discomfort, pain or itchiness
- Have a poor diet or don’t drink enough
- Are recovering from illness or surgery
- Have repetitive behaviours (rocking, rubbing, pressing on objects)
- Have items pressing against the skin for long periods, such as glasses, hearing aids, oxygen masks, wristbands, etc.
Even small things pressing on the same area for too long can cause damage.
Early Warning Signs to Look For
When providing personal care, always check for:
- Discoloured patches (red on lighter skin; purple/blue on darker skin)
- Patches that don’t turn pale/white when pressed
- Skin that feels warm, hard, spongy, or different to surrounding skin
- Complaints of itching or discomfort
These are early signs of a pressure ulcer — they must be reported immediately.
Seek urgent medical help if someone has:
- Red, swollen skin
- Pus or discharge
- Open or concerning skin damage
- Skin that feels unusually cool
- Fast heartbeat
- Confusion
- Severe or worsening pain
- A high temperature (38°C or above)
How to Reduce the Risk
There are lots of simple, everyday steps you can take to help keep someone safe:
✔️ 1. Encourage Regular Movement
- Help the person change position often
- Support gentle stretches
- Encourage walking or sitting in different chairs during the day
✔️ 2. Check Skin Daily
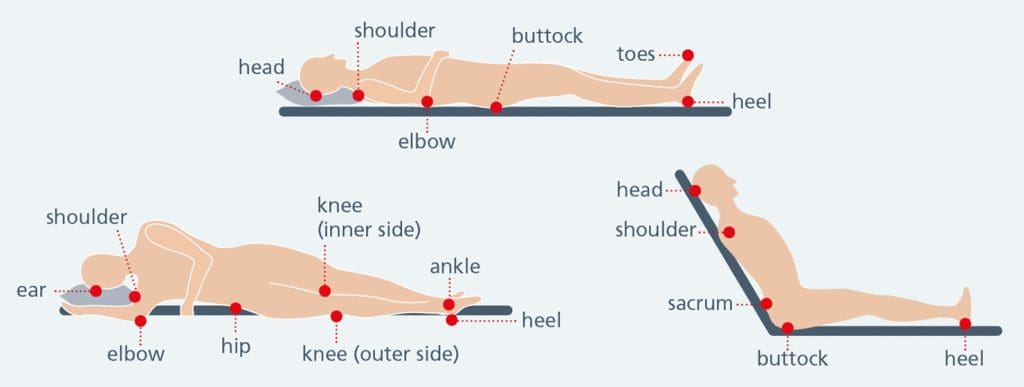
Look especially at bony areas like heels, bottom, hips, elbows and shoulders.
✔️ 3. Support a Healthy Diet
A balanced diet with:
- Enough protein
- Vitamins and minerals, especially Vitamin C and zinc
- Plenty of fluids
If you have concerns, a GP can refer to a dietitian.
✔️ 4. Protect the Skin
- Dry skin thoroughly after washing — no harsh rubbing
- Use gentle movements when repositioning to avoid dragging
- Check whether the person needs prescribed barrier creams or sprays
- Seek guidance from nurses, physios or OTs about slide sheets or equipment
✔️ 5. Help the Person Stop Smoking
Smoking reduces blood flow and increases the risk of pressure ulcers.
Your Responsibilities as a Care Worker
- Know the risk factors and early warning signs
- Record and report any changes in skin condition
- Follow the person’s care plan
- Raise concerns using the correct safeguarding procedures
- Make sure the person and their family have the information they need
Pressure ulcers can often be prevented with good care, teamwork, and early reporting.
Why It Matters
Preventing pressure ulcers is not just clinical — it’s about comfort, dignity, and quality of life.
By checking skin regularly, encouraging movement, and acting early, you can make an enormous difference.
Our Employee Policy is HERE
Follow us on Facebook
Check our other blogs here

